Larva Migrans Interna or Visceral Larva Migrans (VLM)
Parasites
The main causative agents of this disease are the larvae of various roundworm species from domestic and wild animals, for instance, Toxocara canis from dogs and foxes, T. mystax from cats, Baylisascaris procyonis from raccoons as well as roundworm species (Anisakidae) from marine mammals. Toxocariasis and anisakiasis are discussed here as examples from this group. Angiostrongyliosis and dirofilariasis can also be included in this disease category.
Distribution, life cycle, and epidemiology
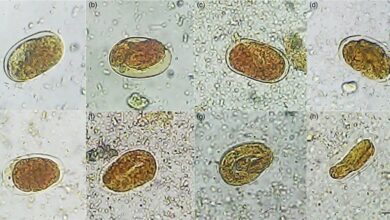
Dogs, cats, and foxes all over the world, especially younger animals, are frequently infected with adult Toxocara roundworms. The parasites live in the small intestine and in most cases produce large numbers of eggs. An infective larva develops in an egg shed into the environment within two to three weeks. Humans are infected by accidental peroral ingestion of infective eggs (geophagia, contaminated foods). Small children run a particularly high risk.
Fairly high levels of contamination of public parks and playgrounds with Toxocara eggs (sandboxes >1–50%) have been found in many cities in Europe and elsewhere. Mean antibody prevalence levels of about 1–8% were measured in healthy persons in Germany, Austria, and Switzerland in serological screening based on a specific ELISA, with figures as high as 30% in some population subgroups.
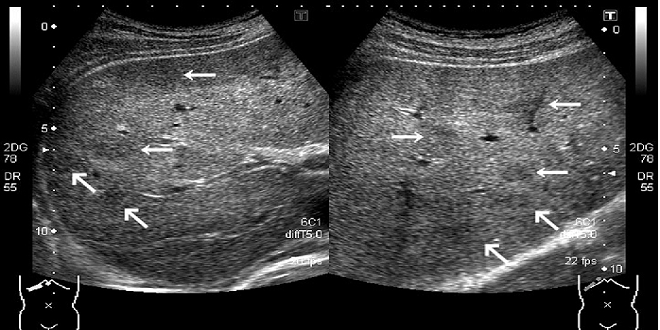
After infection, the Toxocara larvae hatch from the eggshells in the small intestine, penetrate the intestinal wall, and migrate hematogenously into the liver, lungs, CNS, eyes, musculature, and other organ systems. Larvae caught in the capillary filter leave the vascular system and begin to migrate through the organ involved. This results in hemorrhages and tissue destruction as well as inflammatory reactions and the formation of granulomatous foci.
Living larvae are encapsulated in connective tissue in all organs except the CNS, but they can also leave the capsules and continue migrating. The larvae can live for a number of years (at least 10 years in monkeys). The development of adult Toxocara stages in the human intestine is a very rare occurrence.
Clinical manifestations
VLM remains inapparent in most cases. Symptomatic cases are most frequently observed in children aged two to five years. The clinical symptoms depend on the localization and degree of pathological changes and include nonspecific and varied conditions such as eosinophilia, leukocytosis, hepatomegaly, brief febrile episodes, mild gastrointestinal disorders, asthmatic attacks, pneumonia symptoms, lymphadenopathy, urticarial skin changes, central nervous disorders with paralyzes, or epileptiform convulsions. Eye infections are seen in all age groups and present as granulomatous chorioretinitis, clouding of the vitreous body, and other changes. Ocular toxocariasis is often observed without signs of visceral infection.
Diagnosis
Persistent eosinophilia and the other symptoms described above justify a tentative diagnosis. Etiological confirmation requires serological testing for specific antibodies. Highly sensitive and specific techniques are available. Positive zero reactions can be expected four weeks after infection.
Last word
Chemotherapy with albendazole is only indicated in symptomatic cases. Prophylactic measures include control of Toxocara infections in cats and dogs, especially in young animals, and reduction or prevention of environmental contamination with feces of dogs, cats, and foxes, especially on children’s playgrounds.